Patellar Femoral Pain Syndrome (PFPS), also known as runner’s knee, is a common running related issue. The sooner you can manage this condition, the easier it will be to recover and eliminate future problems. Many of my recommended exercises can be adopted as part of a cross training program to prevent PFPS. I will address the many potential causative factors for PFPS and offer advice on how to self-treat this condition.
PFPS can be quite painful and significantly affect a person’s ability to run or move properly. The cause of the pain is often associated with a patellar or knee cap that is tracking in the femoral groove improperly. This can occur for many reasons, but the most common causes are:
- Poor quadriceps strength (particularly the inner or medial quadriceps).
- Poor hip abductor and/or hip external rotator strength.
- Improper foot biomechanics during the single leg stance phase of the gait cycle or the mid foot strike during running. The most common issue within the foot is usually overpronation (when the feet excessively roll inward and cause the knee to roll inward as well during each step). Overpronation is more common among females although males experience it as well. Women may experience overpronation due to the angle of their hips in relation to the knee. A woman’s pelvis is typically a different shape to allow for child bearing. The larger “Q-angle” associated with the hip and knee can cause increased strain on the knee.
PFPS symptoms include:
- The pain will typically increase when going downstairs. In more severe cases, going upstairs is also very painful.
- Pain with squats, lunges, knee extensions, or other plyometric activity.
- Pain typically worsens with prolonged sitting. The longer you sit in one position, the worse the pain becomes.
- Grinding, popping, and cracking are often associated symptoms.
- Pain can be anywhere along the patella (knee cap), but it’s typically associated with anterior knee pain or medial patellar pain.
In many cases, a very thorough warm up may allow you to participate in activity. However, the pain may worsen again later that day or the next day. Seek help or guidance quickly when your pain worsens with activity. For the best result, the treatment plan should be multifactorial.
How to Self-Treat PFPS:
- Improve your quad and your hip strength. Please refer to Patellar Femoral Pain Syndrome Rehabilitation Exercises for my recommended exercise program which is designed to improve quad and hip strength. To improve your quad strength, the emphasis should be on the inner quad known as the vastus medialis oblique (VMO). Weak hip abduction and hip external (lateral) rotation muscles significantly contribute to PFPS. The purpose of the lateral and external rotators of the hip is to prevent internal rotation (rolling inward) of the hip and knee. My recommended exercise program will help to improve your strength.
- Warm up prior to exercise. I recommend that you increase your normal warm up time by at least 10 minutes in order to increase blood flow to the area. This allows for better mobility and also promotes healing as movement is necessary to bring in the nutrients. Use a stationary bike or the rower machine initially to get the muscles warm and the knee joint more lubricated. Then work on moving into a deep squat position multiple times as part of the warm up. You may need to hang onto a beam or a pole to take some pressure off of your knee as you move in and out of the squat.
- Cool down. After performing your exercises, take extra time to cool down and stretch. Use either a stationary bike (at a causal/slower pace) or the rower machine. Both are reduced weight bearing exercises that promote movement and circulation to the knee as well as increasing range of motion (ROM).
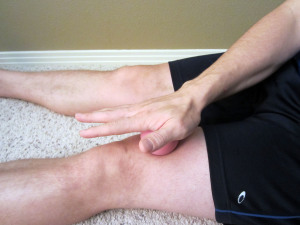
- Self-Mobilize the Tissue. Myofascial release of the quadriceps muscle is an important component in order to relieve the pain and reduce the pressure and tension through the patellar femoral tendon and joint. I tend to use the foam roller for the larger part of the quadriceps. I also use a tennis or lacrosse ball to aggressively work the tissue above the patella. You can use your hand to press the ball in and work it around the tissue. To use the weight of your leg for a more aggressive mobilization, place the ball on the ground and mobilize the tissue with your leg on top of the ball.
- Kinesiological Taping. The purpose of the tape is to assist the patella in its tracking. I have had luck using Kinesio Tape and Mummy Tape brands. There are many other useful taping techniques which utilize different forms of tape. When treating PFPS, I recommend that you apply the tape in a medial direction across the patella approximately 30 minutes prior to exercise or activity. To utilize Mummy Tape, first measure how much of the tape you intend to use. Start from the outside of the knee cap to half way around the leg minus about an inch. Cut the strip, then round the corners on the edge of the tape. This helps the tape to not catch onto clothing. Apply the tape without extra stretch to the first half of the knee cap, then apply between a 50-75% stretch for half of the tape medially toward the inside of the leg. With the last of the tape, apply without a stretch to the inner side of the leg. (You could also utilize Spider tape or KT TAPE.) To visually learn how to apply the tape, please refer to Kinesiological Taping for Patellar Femoral Pain Syndrome. For application and removal tips, please refer to Skin Care with Taping.
- If it hurts, don’t do it! Modify the activity or discontinue it completely. If your knee is hurting when performing a squat, then initially don’t move as deep into the exercise. This would also be true for a lunge position or step up. Modify any exercise as you need to, and don’t compromise technique to complete an exercise. Poor technique will only increase your risk of injury elsewhere.
- Have your gait analyzed while running. Check with your local running store or a physical therapy clinic for a monthly gait analysis clinic. If you’re not a runner, but you’re experiencing pain during other forms of exercise (group aerobics or CrossFit), ask your teacher or coach to analyze your movements during an exercise session. How is your foot striking the ground? Is it rolling in (landing flat footed)? Does your knee rotate inward or stay tracking in line with the foot? Ideally, the knee tracks in line with your second toe. This is important for running as well as squats, step ups, and lunges. If your foot isn’t maintaining a good position during its mid foot strike, a new pair of shoes may be indicated specifically to control pronation. Over-the-counter orthotics can help as well. Superfeet Blue Premium Insoles are available in varying models to help support the arch and heel. They are color coded by model. I wear the blue insoles which are for moderately flat feet. These insoles are very durable. In the past, these insoles have lasted for 1,000 miles through the life cycles of two different pairs of shoes.
- Start a supplement. Many herbs help to reduce inflammation and pain. CapraFlex is one of my favorite supplements. Essentially, it combines an organic glucosamine and chondroitin supplement with other natural herbs which are designed to reduce inflammation. CapraFlex can be taken long term or intermittently to help heal from an injury. I recommend that you try it for 30 days to see if it improves your pain. Another option is Phenocane Natural Pain Management. It combines the following: Curcumin, an herb that reduces pain and inflammation; boswellia, a natural COX2 inhibitor that also reduces pain and inflammation; DLPA, an amino acid that helps to increase and uphold serotonin levels in the brain; and nattokinase, an enzyme that assists with blood clotting and reduces pain and inflammation. (If you are taking blood thinners, please consult with your physician prior to use as the herbs could interact with some medications.)
Patellar Femoral Pain Syndrome can be very painful, but it can be easily self-treated if you handle your pain and symptoms quickly. If you’re not experiencing relief after aggressively managing the symptoms, contact your local physical therapist for an assessment and help in managing PFPS. The American Physical Therapy Association offers a wonderful resource to help find a physical therapist in your area.
Has a specific treatment for PFPS helped you? Which treatments haven’t worked for you? Additional discussion can help others to manage this condition more effectively. Please leave your comments below.
Don’t forget to subscribe to my e-mail list to gain immediate access to My Top 8 Stretches to Eliminate Neck, Upper Back, and Shoulder Pain for step by step exercise instructions and photos!
If you have a question that you would like featured in an upcoming blog post, please comment below or submit your question to contact@thePhysicalTherapyAdvisor.com. Be sure to join our growing community on Facebook by liking The Physical Therapy Advisor!