Q. My knee started hurting about two weeks ago. I have noticed swelling in the back of my knee. It’s painful when I bend or straighten the knee. I looked up the symptoms on WebMD. I think I might have a Baker’s cyst, but I’m not sure what to do now. Your insight would be appreciated, thanks! –Patti
A. Great question, Patti! The symptoms you are describing sound like they may be caused by a Baker’s cyst. Another common diagnosis with similar symptoms would be a meniscus injury. I recommend that you read my previous post on meniscus pain, Q & A: 7 Tips to Get Rid of Knee Pain. Much of the advice will carry over to either condition.
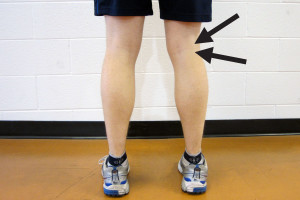
A Baker’s cyst, also known as a popliteal cyst, is a fluid-filled sack that forms in the back of the knee. Synovial fluid from inside of the knee pushes out into a fluid-filled sack in the back of the knee. Sizes of the cysts can wildly vary as do the symptoms. The cyst can typically best be seen when a person is standing. It may or may not be tender to the touch. In fact, you may or may not have any symptoms at all.
Baker’s cyst symptoms include:
- Stiffness or tightness in the back of the knee, thigh, or upper calf.
- Swelling noted behind the knee. If the cyst ruptures, then the swelling may be also be in the lower leg and calf area.
- Pain is most typically described behind the knee, particularly with full flexion (bending) or extension (straightening). A person may also experience pain in the upper calf or back of the thigh.
- Another common complaint is pain when sitting due to the chair touching or rubbing the area behind the knee (known as the popliteal space).
It is not always entirely known why a Baker’s cyst will develop. In my clinical experience, I have seen them form for the following reasons:
- Rheumatoid arthritis (RA)
- Osteoarthritis (OA)
- Recent knee injury or post knee surgery
- Poor lower leg biomechanics, which can lead to other forms of knee pain in addition to a Baker’s cyst.
Baker’s cysts should be diagnosed by a medical doctor. Medical treatment of the cysts usually involves a course of anti-inflammatory medication (orally), a cortisone injection, aspiration of the fluid by utilizing a needle, and/or surgical removal. The good news is that often a Baker’s cyst will typically resolve on its own if you just give it time. Rest and treat any symptoms you may be experiencing.
Physical therapy may also be indicated, particularly if the cyst formed due to osteoarthritis pain, recent knee injury/trauma/surgery, or due to poor lower extremity biomechanics. In most cases, I have witnessed Baker’s cysts successfully and conservatively treated by both a physical therapist and a medical physician who are working together to address the issue.
The rehabilitation for a Baker’s cyst is very similar process to treating meniscus pain. The following 10 tips will help you to rehabilitate your knee. You should experience improvement of your symptoms within in a few of weeks or less when initiating this program. Depending on the severity, it could take longer for a full recovery. If your pain continues or worsens, then additional assessment and follow up is likely needed.
10 Tips on How to Self-Treat a Baker’s Cyst:
1. Rest. Initially, take extra time to rest the painful area. The pain and swelling has likely worsened due to a change in activity level. If the pain is more severe, you may choose to use a cane or a crutch initially to take weight off of the knee.
2. Ice. Apply ice to the knee and behind the knee in particular. The rule of thumb is to ice no more than 20 minutes per hour. Do not place the ice directly against the skin especially if you are using a gel pack style Cold Pack. Individuals with poor circulation or impaired sensation should take particular care when icing. A bag of frozen peas can be ideal in this situation.
3. Compression. Compression helps to prevent and decrease swelling. Swelling can cause increased pain and slow the healing response. Limit it as much as possible. You could utilize a common ACE bandage wrap or you could purchase a pair of mild over-the-counter compression socks. If you utilize a compression sock, it will need to be at least thigh high like these Jobst Relief Therapeutic Thigh High Stockings. Do not use a knee high version–you may make the swelling and pain worse. Do not apply any compression too tightly as it could cause numbness or tingling in the leg, foot, or toes.
4. Taping Techniques. Kinesiological style taping has been proven to be effective in reducing inflammation. Due to the location of the swelling, you will need help from someone trained in the specific style of kinesiological taping. Many physical therapists (PTs), athletic trainers (ATCs), or chiropractors have training in these techniques. Learn How to apply Kinesiology Tape for a swollen (edema) Knee Joint by watching this YouTube video that demonstrates the proper technique. (However, the taping would be on the back side of the knee, not on the front as shown.) I have had luck using the KT TAPE, RockTape Kinesiology Tape, and Mummy Tape brands. The technique is fairly basic, so your spouse or a friend may be able to apply it for you.
5. If it hurts, don’t do it! Modify the activity or discontinue it completely. If your knee is hurting when performing a squat, then initially don’t move as deep into the exercise. This would also be true for a lunge position or step up. Modify any exercise as you need to, and don’t compromise technique to complete an exercise. Poor technique will only increase your risk of injury elsewhere or make the knee more painful and irritated.
6. Warm up prior to exercise. I recommend that you increase your normal warm up time by at least 10 minutes in order to increase blood flow to the area. This allows for better mobility and also promotes healing as movement is necessary to bring in the nutrients. Use a stationary bike or the rower machine initially to get the muscles warm and the knee joint more lubricated.
7. Improve your Range of Motion (ROM). The goal of the rehabilitation program is to regain full pain free ROM. This can be accomplished many ways. Perform heel slides by lying on your back and sliding your heel toward your buttocks. Riding the stationary bicycle can be helpful, too. Remember, the major goal is to regain full pain free ROM. If you experience muscle tightness and soreness, I recommend using a foam roller to assist with any myofascial symptoms. To learn how to use a foam roller, please refer to Foam Rolling for Rehabilitation. Do not use the foam roller directly behind the knee.
8. Work on strengthening. The primary goal of a strengthening program is to work on quadriceps and glut medius (hip abduction) strengthening. These areas are commonly weak which can lead to poor knee biomechanics and cause pain and instability. Weight lifting is an appropriate choice, but you may have to initially limit your range of motion (ROM). Most of my clients begin on a non-weight bearing program, then progress to partial weight bearing, and eventually, full weight bearing. The more severe the symptoms, the longer it will take for an individual to progress to more difficult exercises.
To initiate a physical therapy program, please refer to Baker’s Cyst Rehabilitation Exercises. This exercise guide is designed to address the muscles that I find to be the weakest in most individuals. The exercises are listed from easiest to most challenging and are designed to primarily improve quadriceps and hip strengthening. Start with exercises like a straight leg raise (possibly with an ankle weight) and bridging (either one or both legs). Wall squats holding for time also works well. A Thera-Band Exercise Band can be tied around the thighs above your knees to make your hips more engaged.
Weight training exercises (with machine weights or free weights) should be geared toward general leg strengthening and may include: squats; leg press; hip abduction machine; step ups; dead lifts; and straight leg dead lifts. If further instruction is needed, search YouTube to watch the proper technique for a specific exercise. If full ROM is causing an increase in your pain, then you need to stay within your pain free limit as you work on the ROM separately from weight training.
Initially, you will likely need to taper down your activities. The speed at which exercise is performed while in group exercise classes is typically too fast for an individual who is properly and safely exercising his/her knee during a rehabilitation and recovery phase. You can still participate in group exercise classes or CrossFit WODs (Work out of the Day), but your specific knee program should be separate from any group structured activity. You will need to modify some of the activities performed in your structured class to avoid further pain.
9. Cool down. After performing your exercises, take extra time to cool down and stretch. Use either a stationary bike (at a causal/slower pace) or the rower machine. Both are reduced weight bearing exercises that promote movement and circulation to the knee as well as increasing ROM.
10. Add a joint supplement. If you are experiencing osteoarthritis pain, you may want to consider adding a glucosamine and chondroitin supplement. CapraFlex is my preferred supplement for knee related injuries. I have recommended this supplement for years as my clients have had successful outcomes with use. It has also assisted me in recovery from my many injuries. Essentially, it combines an organic glucosamine and chondroitin supplement with other natural herbs which are designed to reduce inflammation. CapraFlex can be taken long term or intermittently to help heal from an injury. I recommend that you try it for 30 days to see if it improves your knee pain, but do not use it in combination with other traditional anti-inflammatory medications. If you are under the care of your physician, please inform him/her that you are taking this medication. (If you are taking blood thinners, please consult with your physician prior to use as the herbs could interact with some medications.)
In most cases, you should expect a complete resolution of your symptoms upon completion of the rehabilitation process. To prevent the condition from re-occurring, address any ROM or mobility restrictions as well as any weak areas that are causing altered lower leg biomechanics.
If your symptoms and pain continues or worsens after two to three weeks of rehabilitation, please seek additional assistance from your physician or a qualified physical therapist. The American Physical Therapy Association offers a wonderful resource to help find a physical therapist in your area. In most states, you can seek physical therapy advice without a medical doctor’s referral (although it would be a good idea to seek your physician’s opinion as well).
Thank you, Patti, for your question. I hope these 10 tips will help you to rehabilitate your knee and recover quickly!
Which treatments for knee pain are the most effective for you? Please share any recommendations that you may have by leaving your comments below.
If you have a question that you would like featured in an upcoming blog post, please comment below or submit your question to contact@thePhysicalTherapyAdvisor.com. Be sure to join our growing community on Facebook by liking The Physical Therapy Advisor!
Disclaimer: The Physical Therapy Advisor blog is for general informational purposes only and does not constitute the practice of medicine or other professional health care services, including the giving of medical advice. No health care provider/patient relationship is formed. The use of information on this blog or materials linked from this blog is at your own risk. The content of this blog is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Do not disregard, or delay in obtaining, medical advice for any medical condition you may have. Please seek the assistance of your health care professionals for any such conditions.