Cervicogenic headaches are a certain type of headache in which the head pain is specifically caused by an issue in the cervical spine. Cervicogenic pain is often a trigger for other types of headaches, such as migraines or tension headaches. As a physical therapist, I find it more effective to classify cervicogenic headaches separate from tension headaches. Tension and cervicogenic headaches may be treated similarly, but in many cases, it depends on the actual dysfunction present.
Cervicogenic headaches are almost always mechanical in nature. This means that there is a structural or mechanical cause in the neck which is leading to the headache pain. Since the trigger is mechanical, these headaches can come on very suddenly with certain movements and can also be reduced or eliminated quickly if the correct movements can be initiated. When the cervical spine is the cause of the pain, you may experience cervical pain, headache pain, and other correlated or referred pain in your upper back or down your arms (even to your fingers).
Cervicogenic Headache Symptoms include:
- Pain in the front of your head, behind your eyes or side of your head.
- Pain which begins from your neck and extends to between your shoulder blades or upper shoulders.
- Pain which is exacerbated or changed by certain neck movements or neck positions.
- Pain which is triggered by pressure applied to the upper part of the neck near the base of the skull (known as the suboccipital area) or in the upper trapezius area.
- Pain down one or both arms and can be felt as far as your fingers.
- Stiff neck.
- Blurred vision.
- Nausea, vomiting, and/or dizziness.
Potential Causes for Cervicogenic Headaches
There are plenty of reasons why one might develop cervical derangements or dysfunction. Examples include: motor vehicle accidents; sports; falls; sleeping on a poorly fitting pillow; poor posture (especially when texting); and/or carrying items that are too heavy (such as a backpack). Chronically sustained non-symmetrical postures, stress, and/or a sedentary lifestyle are also potential causes.
The actual pain generating structures of the neck (listed below) also vary wildly and can be difficult to pinpoint.
- Nerve related injury or pain
- Muscle spasms
- Trigger points
- Facet joint dysfunction
- Cervical mal-alignments
- Cervical disc issues
- Postural dysfunction
Cervicogenic pain and headaches tend to be more common in women than men. In general, women experience this due to an anatomical difference. Men tend to have more muscular necks while women tend to have more long and slender necks with less muscle to provide support to the head (meaning that there is less muscle strength for support).
Treatment for Cervicogenic Headaches
In cases of mechanical pain, you should be able to alter and change your neck or headache pain within a short period of time. The first step is to establish a directional preference by identifying a pattern to the pain.
Which head motions change or alter your neck or headache pain? Does the pain get worse or does it improve when you turn your head? What happens when you look up, look down, slouch or sit up straight? What happens when you repeat this movement?
Determine how your pain responds. If it spreads away from the spine and down into the upper back or arm, beware that you are moving in the wrong direction. Stop that particular movement, and instead try the opposite direction.
In my experience, most episodes of cervical and headache pain tend to respond better to cervical extension biased movements and improvements in posture. Often, gaining extension in the thoracic spine is also critical to treatment.
In order to determine if extension biased (cervical retraction or extension) movements help you, I recommend starting with this exercise (as shown below). Sit up straight, and retract your chin straight back. Repeat 10-20 times.
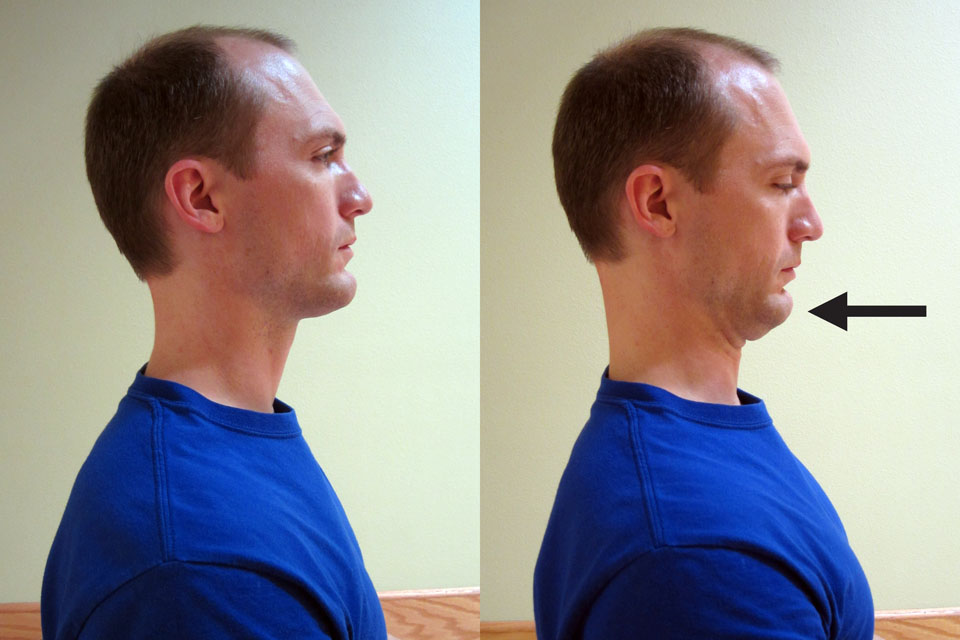
Carefully monitor symptoms for peripheralization or centralization. The rule of thumb for movement: If the pain worsens by spreading peripherally down the arm into the hand, fingers, down into the shoulder blade/upper back or the headache is worsening, then the condition is worsening. Stop that activity. If the pain centralizes and returns back toward the cervical spine, and the headache pain improves (even if the pain in the neck worsens slightly), then keep moving as the condition is actually improving.
If you are unable to help or change the pain in any way, then you may need assistance from a medical provider. For a thorough discussion and an excellent treatment resource, please refer to Treat Your Own Neck by Robin A. McKenzie.
Other Treatments for Cervicogenic Headaches:
- Exercise. A primary treatment modality and prevention technique is exercise. Exercise in general has been shown to be beneficial in treating and preventing cervical pain and headaches. However, a specific exercise program designed to maintain cervical and thoracic mobility and strength should be the main portion of your treatment. Focus on your thoracic mobility (particularly, into extension). Work on cervical stabilization exercises that involve the muscles that support your head and neck.
- Focus on your posture. Poor posture is a bane of modern society. The most common example of poor posture is a forward head with rounded shoulders. This causes excessive muscular tension throughout the cervical spine, upper trapezius region, and mid-thoracic area. Over time, this also leads to muscle weakness and/or dysfunction in the cervical spine and upper thoracic area. Proper posture allows for the optimal alignment of your spine. Neurologically speaking, this allows for your muscles to down regulate by reducing tension. Poor posture is almost always associated with muscle knots and trigger points. My Top 8 Stretches to Eliminate Neck, Upper Back, and Shoulder Pain is a downloadable .pdf file with my recommended stretches and exercises to address posture. These simple exercises (with complete instructions and photos) will help you to improve poor posture and can be performed at home.
DOWNLOAD NOW: My Top 8 Stretches to Eliminate Neck, Upper Back, and Shoulder Pain
- Massage. Many trigger points and muscle spasms will refer pain into the head (which causes the headache). It’s important to actively and physically address the muscle tension. This is the time to contact a masseuse, physical therapist, athletic trainer or friend who is skillful in body work and massage to relieve the area in spasm. The specific massage technique to use will vary according to your preference. Massage techniques range from a light relaxing massage to a deep tissue massage or utilization of acupressure points. This can also be an effective prevention strategy.
- Foam roller. The foam roller allows you to perform self-massage and tissue mobilization. The foam roller is a wonderful tool to prevent muscle cramping and spasms. Please refer to the following posts for more information: Foam Rolling For Rehabilitation and 5 Ways to Improve Range-Of-Motion. I highly recommend a foam roller to help aid in your recovery.
- Other self-mobilization tools. Many times, a friend or masseuse isn’t available to assist when you need the help the most. A foam roller cannot effective reach places in the upper back or arms, so other self-mobilization tools may be necessary. You can get creative and use a tennis ball or golf ball, but I like a specific tool called a Thera Cane Massager. This tool allows you to apply direct pressure to a spasming muscle. When held for a long enough period of time, the Thera Cane Massager will usually cause the muscle spasms to release and provide much needed pain relief!
- Magnesium. A deficiency in magnesium is often associated with headache symptoms and can also heighten the pain response. Take magnesium orally (such as Mag Glycinate in pill form) or apply it topically in order to help mediate the pain response.
- Topical agents. Many topical agents can help to decrease and eliminate muscle spasms or mediate the pain response which can help to reduce headache pain. You can apply a small amount of the topical agent directly over the headache pain area if it’s accessible and not near your eyes. (Please use common sense.) You may find that one product works better than another. Some of my favorite products in my medicine cabinet include: Biofreeze Pain Relieving Gel; Arnica Rub (Arnica Montana, an herbal rub); and topical magnesium.
- Magnesium bath. The combination of warm water with magnesium is very soothing and relaxing. Magnesium is known to help decrease muscle pain and soreness. Options include: Epsoak Epson Salt or Ancient Minerals Magnesium Bath Flakes. I find that the magnesium flakes work better, but they are significantly more expensive than Epson salt.
- Acupuncture. I am personally a big fan of acupuncture. It is very useful in treating all kinds of medical conditions. It can be particularly effective in treating headaches, muscle trigger points, muscle cramps, spasms, and pain as it addresses the issues on multiple layers. Acupuncture directly stimulates the muscle by affecting the nervous system response to the muscle while producing a general sense of well-being and relaxation.
- Manual Therapy. A physical therapist or chiropractor can use manual therapy techniques which can be beneficial in reducing pain and addressing some of the mechanical causes. However, manual therapy is a passive treatment. For long term treatment and prevention, an active approach needs to be taken. I would encourage you to perform proper exercises to insure that you have adequate cervical and upper thoracic strength and mobility. Also, address any precipitating factors (such as poor posture).
- Medications. Medications can be an effective short term solution to headache pain, but I strongly encourage you to transition off of medications over time. In some cases, prescription medications may be used initially to help you tolerate the pain as you work toward prevention. Please speak to your physician regarding prescription options.
- Speak with your Physical Therapist (PT) or Physician (MD). If you are suffering with headache and muscle tension/pain, there are options. Please speak to your medical provider to determine if other causes are contributing to the problem. Physical therapy is very good at assisting those suffering with these types of headaches. The American Physical Therapy Association (APTA) offers a wonderful resource to help find a physical therapist in your area. In most states, you can seek physical therapy advice without a medical doctor’s referral (although it may be a good idea to hear your physician’s opinion as well).
Don’t give up hope! Headache pain is difficult to manage, but with proper care most headache pain can be cured or effectively managed. Begin by implementing one or two of these treatment tips, and then assess how well they worked for you. If the technique helped, continue with it and then implement another strategy.
If you suffer from cervicogenic headaches, which treatments have worked the best for you? Please share below.
If you have a question that you would like featured in an upcoming blog post, please comment below or submit your question to contact@thePhysicalTherapyAdvisor.com. Be sure to join our growing community on Facebook by liking The Physical Therapy Advisor!
Disclaimer: The Physical Therapy Advisor blog is for general informational purposes only and does not constitute the practice of medicine or other professional health care services, including the giving of medical advice. No health care provider/patient relationship is formed. The use of information on this blog or materials linked from this blog is at your own risk. The content of this blog is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Do not disregard, or delay in obtaining, medical advice for any medical condition you may have. Please seek the assistance of your health care professionals for any such conditions.
