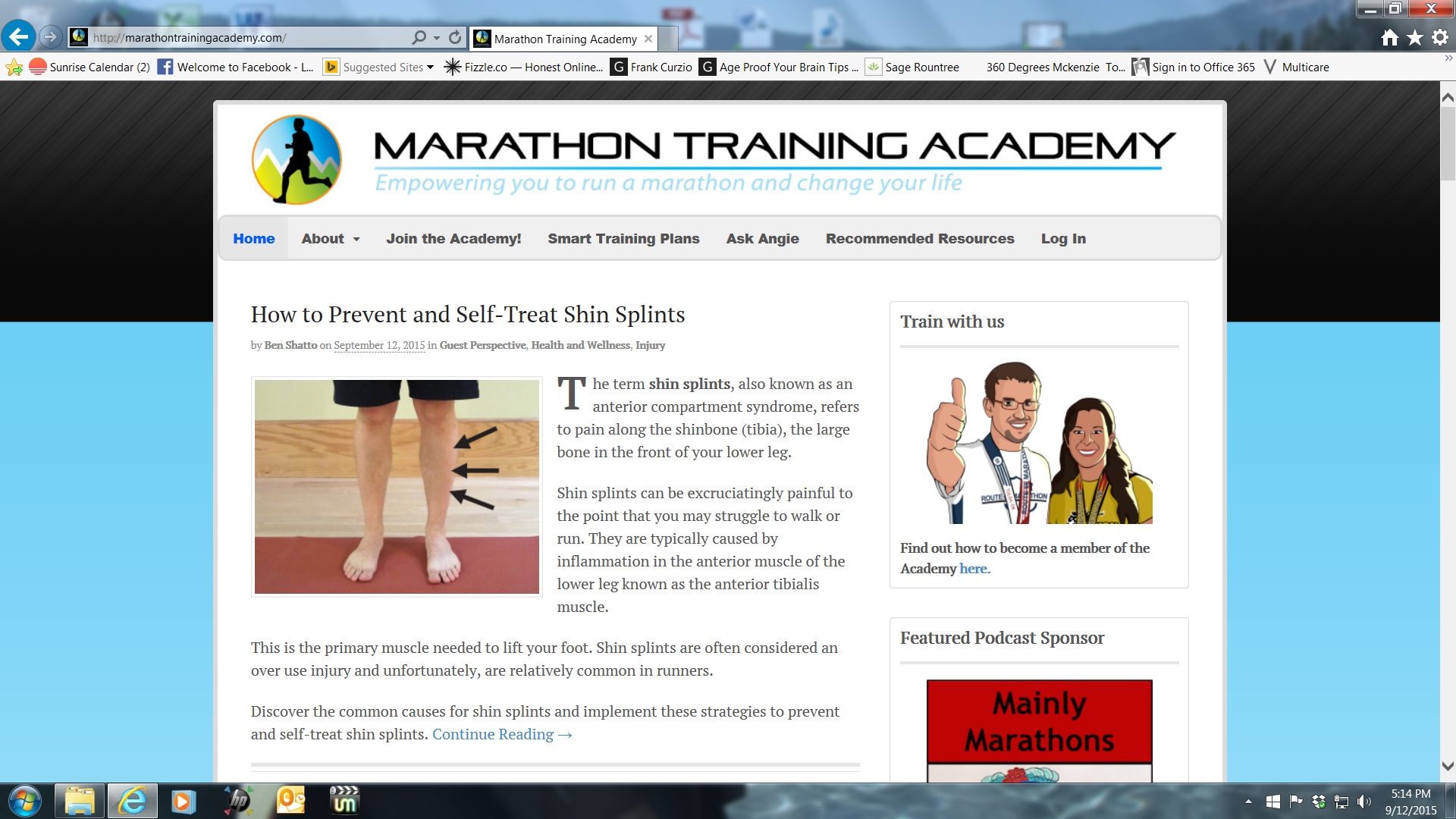
There isn’t a shortage of promising lotions, braces, taping techniques, exercises, and electric modalities when treating knee pain. Many of these fancy options may or may not work to prevent and/or reduce pain. There are many potential reasons for experiencing knee pain. However, an often overlooked cause is the lack of a normal range of motion and tightness in the quadriceps and/or hamstrings. Getting back to the basics can be an integral component to successfully treating knee pain or preventing further injury.
Potential Risk Factors for Knee Pain:
- Poor quadriceps strength (particularly, the inner/medial quadriceps).
- Poor hip abductor and/or hip external rotator strength.
- Prior knee injury.
- Over use.
- Obesity.
- Poor foot biomechanics including overpronation (when the feet excessively roll inward, which causes the knee to roll inward during each step).
- A larger “Q-angle” which is the associated angle between the hip and knee.
- Even anomalies in the shape of one of the bones that make up the knee joint could predispose you to knee pain.
The most obvious (yet rarely talked about) reason for experiencing knee pain directly relates to your range of motion (ROM). In its simplest form, the knee is a hinge joint. It bends and straightens (flexes and extends). If your knee isn’t able to fully bend or straighten because of either excessive quadriceps tightness and/or hamstring tightness, then you’re at an elevated risk for many common knee pain diagnoses including Patellar Femoral Pain Syndrome (PFPS) and Patellar Tendinitis.
Quadriceps Tightness
Poor range of motion in the quadriceps can be associated with a higher risk for developing knee pain. One potential reason for this is that the quadriceps muscle blends into the quadriceps tendon. Eventually it attaches to the patella (kneecap) before becoming the patellar tendon where it attaches to the tibial tubercle on the tibial bone (the main lower leg bone).
Excessive tightness will cause alterations in force and tracking of the patella. This can lead to inflammation and ultimately, pain in or around the structures of the knee (including the patella, quadriceps tendon, patellar tendon, the patellar femoral joint or the infrapatellar fat pad). The following four muscles make up the quadriceps: vastus lateralis; vastus medialis; rectus femoris; and the vastus medialis. The rectus femoris is most likely to be tight as it crosses two joints–both the hip joint and the knee joint. The other muscles only cross one joint–the knee joint.
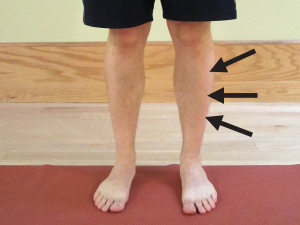
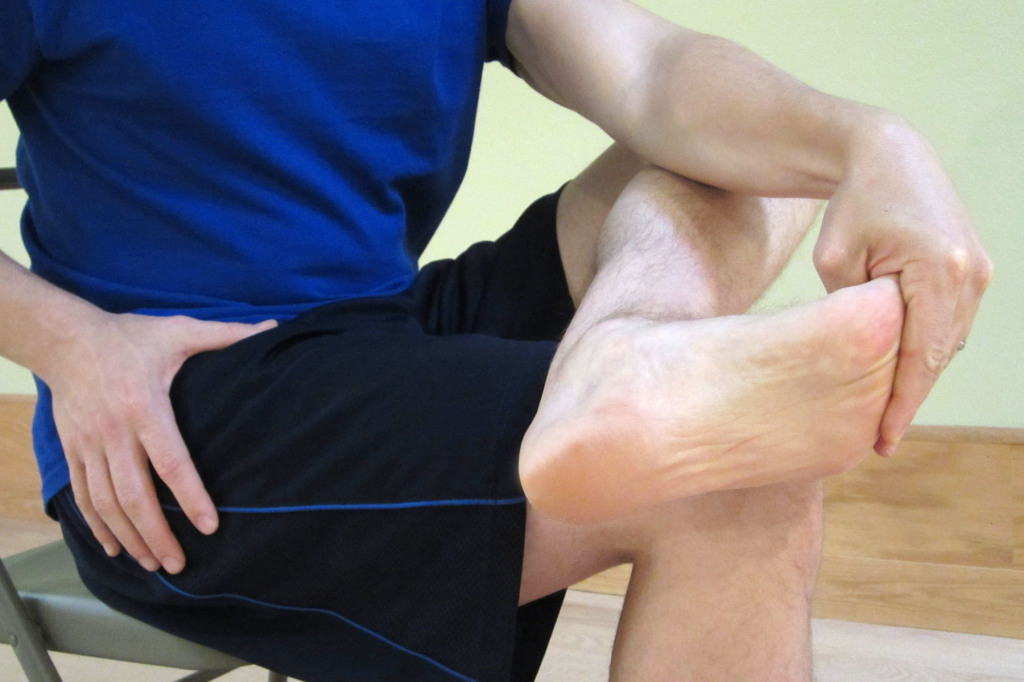
Normal range of motion in the quadriceps will vary from person to person (especially, the older you get or if you have a history of injury). For most healthy and younger to middle aged people, normal range of motion could be defined as the ability to touch your heel to your buttocks with your hip and low back in a neutral (not flexed or extended) position (as demonstrated below).

Regular static stretching and mobilization will help you to improve your range of motion in the quadriceps and ultimately, avoid knee pain.
Static Stretch
Static stretching is best performed post workouts. (Static stretching prior to a work out or activity has been shown to decrease performance.) Hold the following stretch for at least 60 seconds, and perform two to three repetitions.

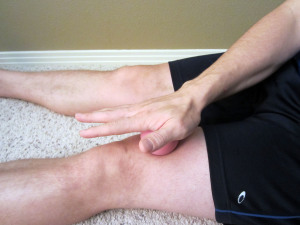
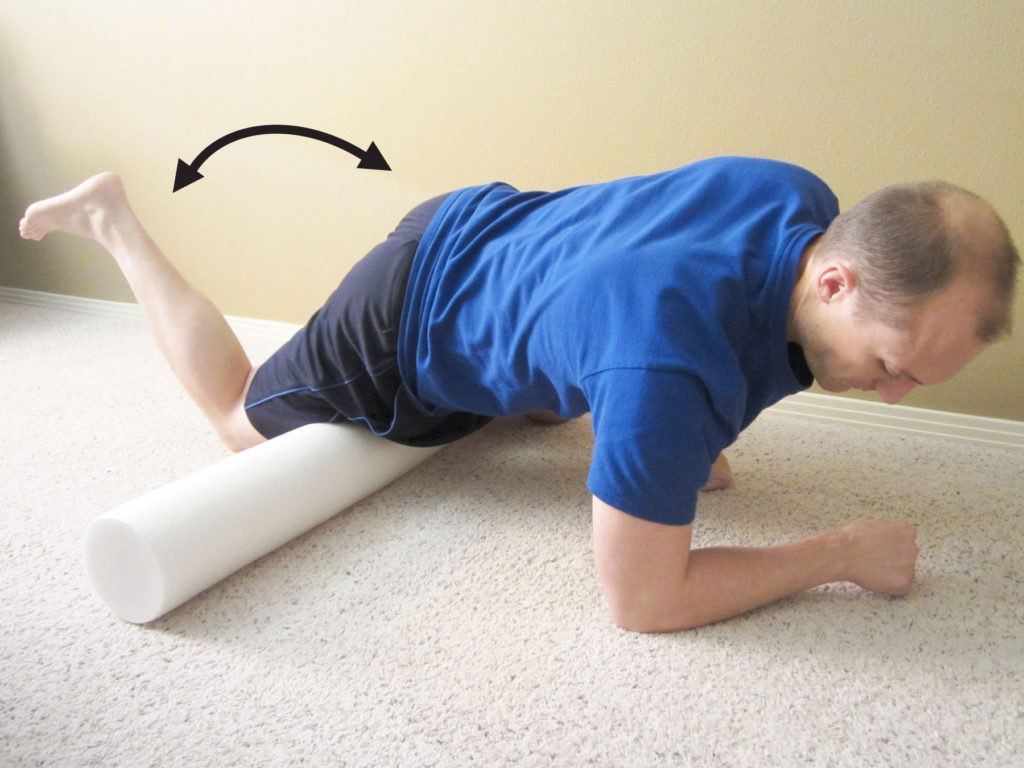
Quadriceps “Tack and Floss” Mobilization
You can use a foam roller to help mobilize the quadriceps while working on your range of motion. Position your upper thigh onto the foam roller. Roll around until you locate a particularly tight and/or restricted area, and then very slowly bend your knee back and forth. If this is painful, do not exceed more than a mild to moderate amount of pain. Perform 1-2 minutes on each leg once per day.
Hamstring Tightness
Hamstring tightness can often restrict full knee extension (particularly, during functional activities). The most common reason for poor hamstring mobility is chronic poor posture while sitting and standing. Most of us sit for a good portion of the day. This results in tight hamstrings and increases your risk for experiencing knee pain as well as low back pain.
Poor range of motion can also be a contributing factor to muscle imbalances. A hamstring that is either too long (over stretched) or a hamstring that is too short and contracted will not generate as much force and strength as a hamstring within its optimal length. The ability for a muscle to contract optimally is dependent on it being at an optimal length. This is known as the length tension relationship.
Many people (women in particular) struggle with adequate hamstring strength in relationship to quadriceps strength. This muscle imbalance can lead to pain and is a major risk factor in suffering an ACL tear. Therefore, one way to insure proper hamstring strength is to insure proper hamstring length.
Hamstring Stretch in Doorway
Static stretching is best performed post workouts. (Static stretching prior to a work out or activity has been shown to decrease performance.) Find a doorway and place one leg on the frame and stretch the opposite leg through the doorway. Try to keep your back with a neutral arch. As your hamstring relaxes, slowly move closer to the wall or doorframe. Hold for at least 1 minute per side, and preferably two repetitions per side.

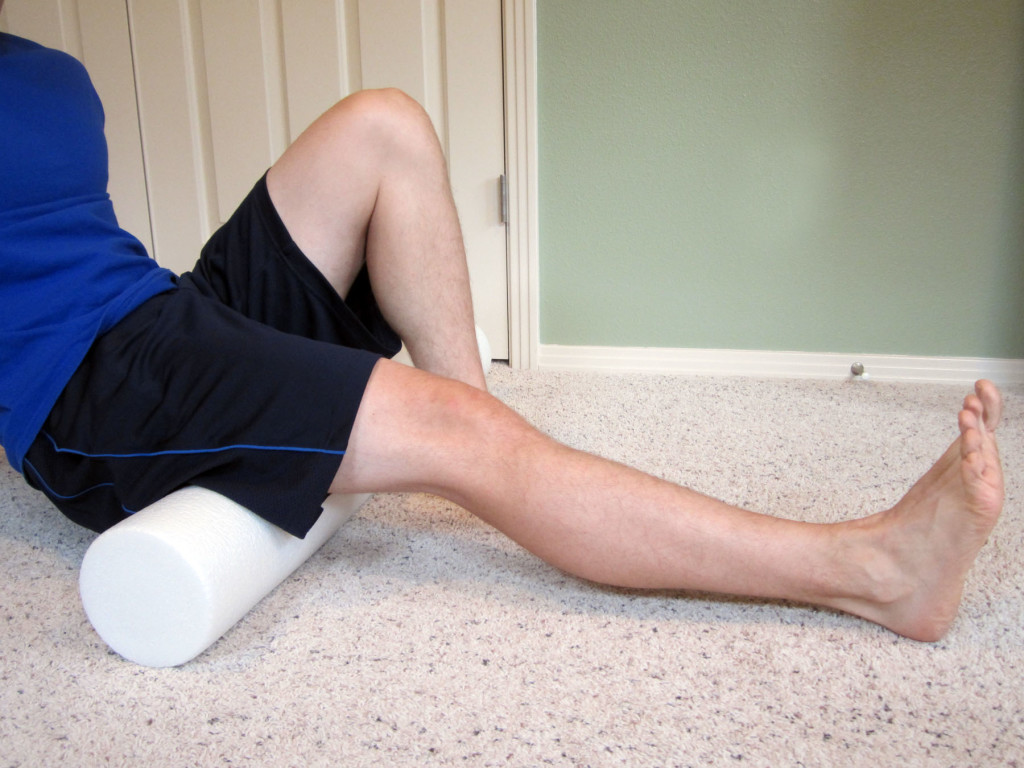
Hamstring Mobilization Using the Foam Roller
Place your leg on the foam roller. Roll your hamstring back and forth on the foam roll. Move slowly and spend extra time on the more painful areas. Be sure to mobilize the entire hamstring and feel free to work on other areas of the leg that feel tight or restricted. If this is painful, do not exceed more than a mild to moderate amount of pain. Perform for 1-2 minutes per leg.
Don’t forget the basics when it comes to self-treating knee pain. Lack of range of motion could be the most simple and obvious reason for why you’re experiencing knee pain. Implement my recommended exercises in order to address any tightness in the quadriceps and/or hamstrings. Getting back to the basics can be an integral component to successfully treating your knee pain and preventing further injury.
If you’re experiencing knee pain, do you think either poor range of motion and/or tightness in your quadriceps and/or hamstrings are causing it? Which strategy can you implement to alleviate your pain and prevent injury? Please share below.
If you have a question that you would like featured in an upcoming blog post, please comment below or submit your question to contact@thePhysicalTherapyAdvisor.com. Be sure to join our growing community on Facebook by liking The Physical Therapy Advisor!